Chong AS, Rothstein DM, Safa K, Riella LV. Minireview on Outstanding Questions in Transplantation: B Cells, Alloantibodies, and Humoral Rejection. Am J Transplant. 2019 Feb 25. doi: 10.1111/ajt.15323. [Epub ahead of print]
Abstract
Over the past three decades, improved immunosuppression has significantly reduced T cell-mediated acute rejection rates, but long-term graft survival rates have seen only marginal improvement. The cause of late graft loss has been under intense investigation, and chronic antibody-mediated rejection (AMR) has been identified as one of the leading causes, thus providing a strong rationale for basic science investigation into donor-specific B cells and antibodies in transplantation and ways to mitigate their pathogenicity. In 2018, the American Society of Transplantation launched a community-wide online discussion of Outstanding Questions in Transplantation and the topic of B cell biology and donor-specific antibodies prevention emerged as a major area of interest to the community, leading to a highly engaged dialogue, with comments from basic and translational scientists as well as physicians (http://community.myast.org/communities/community-home/digestviewer). We have summarized this discussion from a bedside to bench perspective and have organized this review into outstanding questions within the paradigm that AMR is a leading cause of graft loss in the clinic, and points of view that challenge aspects of this paradigm. We also highlight opportunities for basic and translational scientists to contribute to the resolution of these questions, mapping important future directions for the transplant research field. This article is protected by copyright. All rights reserved.
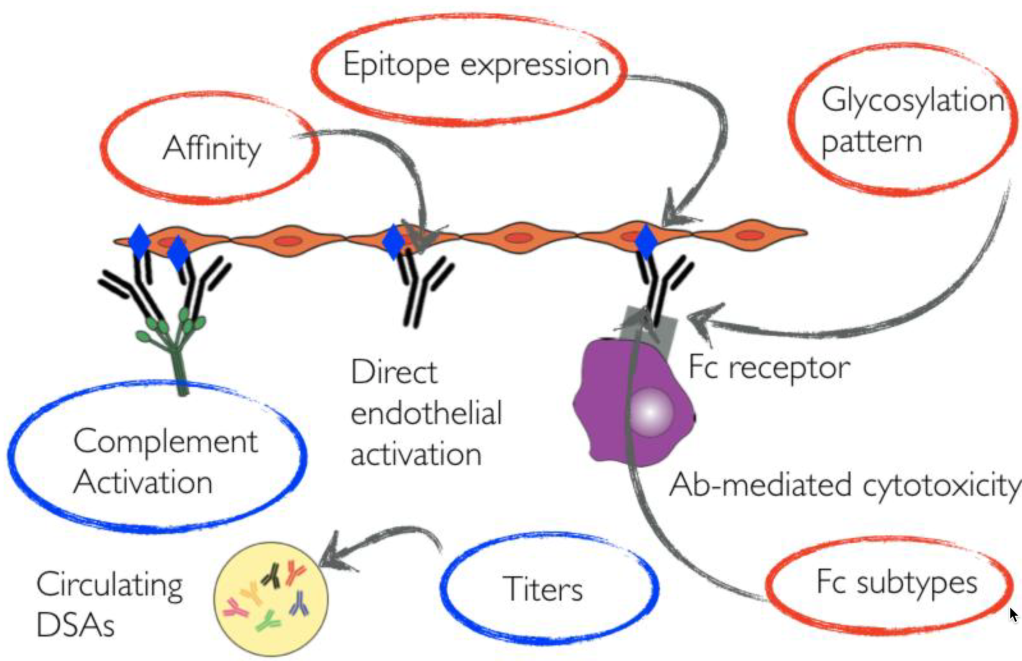
Figure 1. Potential determinants of DSA pathogenicity in the allograft. Routinely assessed DSA characteristics are marked in blue circles, while not routinely performed are marked in red circles.